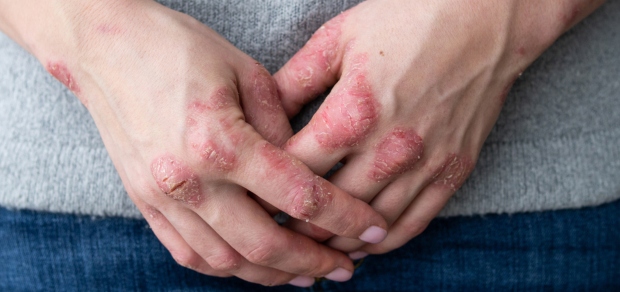
The 5 Most Common Types of Psoriasis: Which One Do You Have?
Worldwide, more than 125 million people have psoriasis, including more than eight million in the United States, according to the National Psoriasis Foundation. But just because your friend, cousin, or coworker has this autoimmune condition doesn’t mean they have the exact same symptoms as you. In fact, there are five main types of psoriasis: plaque, guttate, inverse, pustular, and erythrodermic. And each one comes with a unique set of concerns. Knowing which type you have can help you understand what’s happening with your body so you and your doctor can determine the most effective treatment.
Plaque Psoriasis
A whopping 80 percent of people diagnosed with psoriasis have the most common form: plaque psoriasis. Typically, skin cells take about a month to grow deep in your skin and then rise to the surface. But in plaque psoriasis, cells rise in a matter of days, before they have had a chance to mature. The new cells and existing cells pile up on the surface of the skin, causing raised, red patches covered with a silvery-white buildup of dead skin cells, called plaques. Plaque psoriasis is most often found on the scalp, knees, elbows, and lower back. The plaques, also known as psoriatic lesions, are often itchy or painful and can crack and bleed.
“If only a small area of the body is affected, this type of psoriasis is often treated with topical steroids,” according to M. Laurin Council, M.D., an associate professor of dermatology at Washington University School of Medicine in St. Louis. “Light therapy and systemic treatment, such as biologic medication taken orally or injected, is needed for larger areas of involvement.” Systemic treatments are those that work to surpress an overactive immune system; biologics are a type of systemic treatment that are often injected but are sometimed delivered by an IV infusion.
As far as self-care is concerned, keeping the skin moisturized, applying OTC cortisone cream, and avoiding personal triggers may help people with plaque psoriasis.
Guttate Psoriasis
Guttate psoriasis looks different than the plaques people tend to associate with psoriasis. It appears as small, dot-like lesions. It usually starts in childhood or young adulthood and can be triggered by a strep infection. This is the second most common type, with approximately ten percent of those diagnosed with psoriasis having guttate, according to the National Psoriasis Foundation.
“Because guttate psoriasis is sometimes the body’s reaction to a strep infection, the first step is treating the infection,” explains Council. Once the infection clears up, the psoriasis can be treated. With guttate psoriasis, the type of treatment usually depends on how much of the body is affected, she says.
Inverse Psoriasis
Inverse psoriasis can be particularly uncomfortable since it’s found where skin touches skin, such as behind the knee or in the armpit or groin area. The lesions are very red, shiny, and smooth. Many people with inverse psoriasis also experience a flare of a different type of psoriasis at the same time. Treatments include topical medications, systemic medications, or a combination of both, says Council.
Pustular Psoriasis
People with pustular psoriasis experience flare-ups of white pustules (blisters filled with noninfectious pus) surrounded by red skin. These flares often appear quickly. You may get them on any part of the body, but they’re most often found on the hands or feet. If you have pustular psoriasis, work with your doctor to find medication that will ease your irritation. “It is typically treated with light therapy or systemic therapy,” according to Council.
Erythrodermic Psoriasis
Erythrodermic psoriasis is the most severe form of psoriasis, and thankfully it’s rare. It’s characterized by widespread, fiery redness over most of the body; severe itching; and, pain. Only about three percent of people diagnosed with psoriasis develop this type sometime in their life—it most often occurs in those with unstable plaque psoriasis.
During an erythrodermic outbreak, skin can come off in sheets. It is life-threatening, so if you think you are experiencing symptoms, seek immediate medical attention.
Where Severity Comes into Play
When finding the best treatment for your psoriasis, identifying the type of psoriasis isn’t the only step that will help. In fact, knowing the severity level may be even more crucial when choosing a treatment plan, says Council. Not sure how severe yours is? Typically, doctors diagnose the severity of psoriasis this way:
- Mild psoriasis: Lesions cover less than three percent of the body surface.
- Moderate psoriasis: Lesions cover three to 10 percent of the body.
- Severe psoriasis: More than 10 percent of the body is covered.
When determining the severity of your psoriasis, also consider your quality of life. Even if lesions only cover a small part of your body surface, the condition can still negatively affect your day-to-day. For example, if it is particularly painful, you may find it very difficult to carry out daily activities and your doctor may upgrade your severity level.
“Small areas can be treated with topical medications where large areas of involvement are best treated with systemic (oral or injectable) medications or phototherapy,” says Council.
Your doctor may even prescribe a combo of therapies to help ease your symptoms.
“The systemic medications are highly effective. They’re available as an oral medication or injection and do a great job at minimizing the disease,” explains Council. “Any residual affected areas can be treated with topical medications.” However, some people do report side effects such as nausea and diarrhea, and there may be an increased risk of infection while taking systemic medications.
If psoriasis symptoms are interfering with daily activities or are bothersome, you should seek medical attention, advises Council. Your doctor can work with you to find the treatment that will be most effective for you.
Because of the sheer number of options available to treat psoriasis, there is usually something that will work to clear most of a patient’s symptoms, she adds.
Preventing Flares
While you can’t completely cure your psoriasis, there are ways you can control and manage it. First, recognize the factors that can trigger your symptoms. Common triggers include:
- Stress
- Dry skin
- Skin irritations
- Cold weather
- Smoking
- Infections (such as strep throat or the common cold)
- Diseases that weaken the immune system
- Certain medications, such as beta-blockers for high blood pressure
At-home care can help prevent flare-ups. Some things you can do include:
- Moisturize, moisturize, moisturize.
- Keep your skin covered when the air is cold and dry.
- Use a humidifier at home.
- Use stress-relieving techniques, such as yoga, deep breathing, or meditation.
- Try to avoid cuts, scrapes, and skin infections.
- Limit alcohol consumption.
- Follow a healthy diet.
- Exercise regularly.
Also, if you’re taking medications for other health conditions—even over-the-counter drugs—talk to your doctor about whether those can increase flare-ups, and if you can safely substitute other medications.
Complications of Psoriasis
“Psoriasis is not typically thought of as a dangerous condition,” explains Council. “But it is associated with other medical conditions, such as metabolic syndrome (obesity, cardiovascular disease, hypertension, and high cholesterol), which are considered more dangerous.” People with severe psoriasis are 58 percent more likely to have a significant cardiac event, such as a heart attack, and some research suggests that cardiovascular disease is the leading cause of death in those with psoriasis. Other conditions associated with psoriasis include cancer, Crohn’s disease, depression, osteoporosis, uveitis (a type of eye inflammation), liver disease, and kidney disease.
Up to 30 percent of people with psoriasis develop psoriatic arthritis, according to Cleveland Clinic. The most common symptoms of psoriatic arthritis include stiffness, pain, and swelling in one or more joints.
Because of the increased health risks, if you have psoriasis, it is crucial to maintain a healthy weight, have regular checkups, monitor your blood pressure, and exercise regularly. These steps can help you live a healthy life and help you manage your condition.
You May Also Like:
Want to Read More?
Access all of Twill Care’s content, community, and experts for free!
Already a member? Login
Want to Read More?
Access all of Twill Care’s content, community, and experts for free!
sign UP For FreeAlready a member? Login

